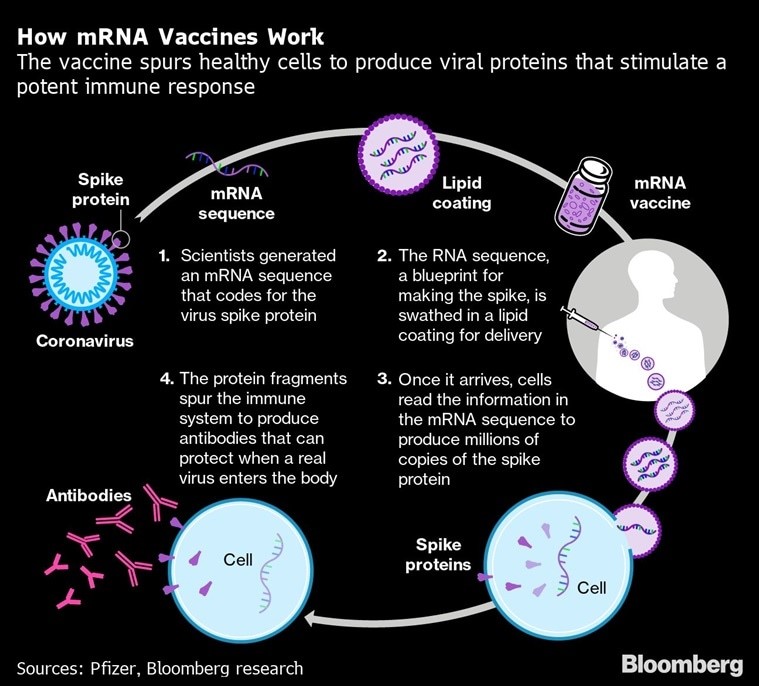
Recently, 2023 Prize in Physiology or Medicine was awarded to Katalin Karikó and Drew Weissman for their discoveries concerning nucleoside base modifications that enabled the development of effective mRNA vaccines against COVID-19.
|
Nobel Prize in Medicine 2023 |
|
|
Advantages |
Disadvantages |
|
They are easy to design, speed and lower cost of production. They only need the genetic code and is possible to update vaccines to emerging variants and use them for a variety of diseases. |
They may require ultra-cold storage before distribution. They need to be frozen from -90 degree Celsius to -50 degree Celsius. |
|
They induce both cellular and humoral immunity. |
They may cause adverse reactions in people susceptible to an autoimmune response. |
|
They do not interact with the genomic DNA. |
They may have unknown long term effects. |
Chimeric antigen receptor T cells (CAR-T) therapy is a form of cancer immunotherapy currently in use around the world to treat certain forms of leukaemia. It uses immune cells called T cells that are genetically altered in a lab to help them locate and destroy cancer cells more effectively.