What is the issue?
- The role of ‘silent spreaders’ in the coronavirus pandemic highlights the significance of testing. Click here to know more on this
- In this backdrop, here is a look at the two types of tests to detect the virus infection - RT-PCR based and the antibody based.
How does the Coronavirus express itself?
- A virus is a microscopic package of genetic material (either DNA or RNA) surrounded by a molecular envelope.
- Some viruses such as the coronavirus (SARS-Cov2) only contain RNA.
- This means that they rely on infiltrating healthy cells to multiply and survive.
- Once inside the cell, the virus uses its own genetic code to take control of and ‘reprogramme’ the cells to make them become virus-making factories.
What is the RT-PCR method in testing?
- Real time RT-PCR (reverse transcription–polymerase chain reaction) is now one of the most accurate laboratory methods for detecting, tracking, and studying the coronavirus.
- RT-PCR is a nuclear-derived method for detecting the presence of specific genetic material from any pathogen, including a virus.
- It uses markers to detect the presence targeted genetic materials.
- Originally, radioactive isotope markers were used.
- Subsequent refining has led to the replacement of the isotopic labelling with special markers, most frequently fluorescent dyes.
- With real time RT-PCR, scientists can see the results almost immediately while the process is still ongoing. [Conventional RT-PCR only provides results at the end.]
What is the principle behind?
- In order for a virus like the coronavirus to be detected early in the body, using real time RT-PCR, scientists need to convert the RNA to DNA.
- This is a process called ‘reverse transcription’.
- They do this because only DNA can be copied - or amplified - which is a key part of the real time RT-PCR process for detecting viruses.
- Scientists amplify a specific part of the transcribed viral DNA hundreds of thousands of times.
- By this amplification, instead of trying to spot a minuscule amount of the virus among millions of strands of genetic information, scientists have a large enough quantity of the target sections of viral DNA.
- This facilitates in the accurate confirmation that the virus is present.
How does RT-PCR work in Coronavirus case?
- A sample is collected from parts of the body where the coronavirus gathers, such as a person’s nose or throat.
- The sample is treated with several chemical solutions.
- This remove the substances, such as proteins and fats, and extracts only the RNA present in the sample.
- This extracted RNA is a mix of a person’s own genetic material and, if present, the coronavirus’ RNA.
- The RNA is reverse transcribed to DNA using a specific enzyme.
- Then, additional short fragments of DNA are added that are complementary to specific parts of the transcribed viral DNA.
- Some of the added genetic fragments are for building DNA strands during amplification.
- The others are for building the DNA and adding marker labels to the strands, which are then used to detect the virus.
- These fragments attach themselves to target sections of the viral DNA if the virus is present in a sample.
- The mixture is then placed in a RT-PCR machine.
- The machine cycles through temperatures that heat and cool the mixture to trigger specific chemical reactions.
- These reactions then create new, identical copies of the target sections of viral DNA, and the cycle repeats over and over to continue copying.
- [Each cycle doubles the previous amount: two copies become four, four copies become eight, and so on.
- A standard real time RT-PCR setup usually goes through 35 cycles.
- So, by the end of the process, around 35 billion new copies of the sections of viral DNA are created from each strand of the virus present in the sample.]
- As new copies of the viral DNA sections are built, the marker labels attach to the DNA strands and then release a fluorescent dye.
- This is measured by the machine’s computer and presented in real time on the screen.
- The computer tracks the amount of fluorescence in the sample after each cycle.
- When the amount goes over a certain level of fluorescence, this confirms that the virus is present.
- Scientists also monitor how many cycles it takes to reach this level in order to estimate the severity of the infection.
- [The fewer the cycles, the more severe the viral infection is.]
- Advantages - This technique is highly sensitive and specific and can deliver a reliable diagnosis as fast as 3 hours, though usually laboratories take on average between 6 to 8 hours.
- Comparatively, real time RT-PCR is significantly faster and has a lower potential for contamination or errors.
- This is because the entire process can be done within a closed tube.
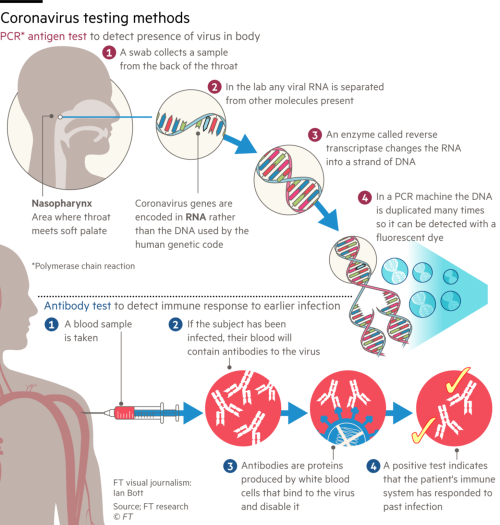
What is the anti-body test?
- The antibody test is based on a biological phenomenon.
- In response to entry of any ‘foreign invader’ (virus, in this case), antibodies are generated by the body's own immune system.
- Such antibodies are specific to that invader.
- Therefore, detection of specific antibodies in a blood sample may indicate that 'at some point', that individual is exposed to that invader.
What are the drawbacks in anti-body test?
- Unlike DNA, antibodies cannot be copied in a test tube, and therefore, this test is generally less sensitive than PCR.
- Also, the human body takes some time to generate antibodies after it is exposed to an invader.
- Antibodies continue to be present in the blood for some time even after the invader is completely eliminated from the body and there are no clinical symptoms.
- [The human body is capable of generating immunological memory after first infection.
- So, the next time, if same invader re-enters, the body is better prepared to eliminate the infection (a principle behind all vaccinations).
- In some cases, this memory (which is typically called “immunity”) is life long; in other cases, it is short termed.]
Why are both tests relevant now?
- Clearly, the controversy of one test over the other is misplaced; both are important, but their purposes are different.
- RT-PCR is the confirmatory test to be done when someone comes with clinical symptoms.
- The same test will certify if the patient is fully recovered or not.
- RT-PCR will give an idea if people within the immediate proximity of a newly-confirmed patient are infected by the virus.
- However, in this case, the first negative result does not completely rule out lack of infection.
- Therefore, quarantine/isolation of these people (who were in proximity with patient) is essential.
- On the other hand, the vast majority (by some estimates 70-80%) would have sub-clinical infection (they have never shown any symptoms).
- So, in this case, the antibody test will give data on how many people are exposed to the virus at some point of time.
- This would be essential to estimate the extent of virus spread in the community and to respond appropriately.
Source: The Print, IAEA
